Rectal Vaginal Fistula Treatment Market Size, Share, and Trends Analysis Report
CAGR :

| Market Size 2023 (Base Year) | USD 533.65 Million |
| Market Size 2032 (Forecast Year) | USD 956.61 Million |
| CAGR | 6.7% |
| Forecast Period | 2024 - 2032 |
| Historical Period | 2018 - 2023 |
Rectal Vaginal Fistula Treatment Market Insights
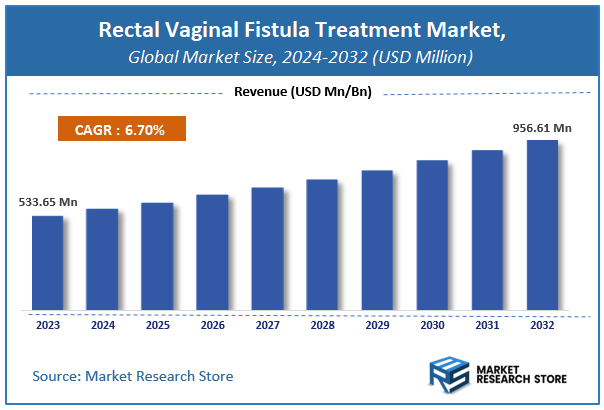
According to Market Research Store, the global rectal vaginal fistula treatment market size was valued at around USD 533.65 million in 2023 and is estimated to reach USD 956.61 million by 2032, to register a CAGR of approximately 6.7% in terms of revenue during the forecast period 2024-2032.
The rectal vaginal fistula treatment report provides a comprehensive analysis of the market, including its size, share, growth trends, revenue details, and other crucial information regarding the target market. It also covers the drivers, restraints, opportunities, and challenges till 2032.
To Get more Insights, Request a Free Sample
Global Rectal Vaginal Fistula Treatment Market: Overview
Rectal vaginal fistula (RVF) is an abnormal connection between the rectum and the vagina, resulting in the involuntary passage of gas or feces through the vaginal canal. This condition often arises due to complications during childbirth, pelvic surgeries, Crohn’s disease, radiation therapy, or pelvic cancers. It can severely affect a woman’s quality of life, causing physical discomfort, infections, embarrassment, and emotional distress. Treatment typically involves surgical repair, which may vary based on the size, location, and underlying cause of the fistula. In some minor cases, non-surgical methods like dietary adjustments and antibiotics may be tried, but surgery is usually the definitive solution—often using transvaginal, transanal, or abdominal approaches depending on the complexity.
Key Highlights
- The rectal vaginal fistula treatment market is anticipated to grow at a CAGR of 6.7% during the forecast period.
- The global rectal vaginal fistula treatment market was estimated to be worth approximately USD 533.65 million in 2023 and is projected to reach a value of USD 956.61 million by 2032.
- The growth of the rectal vaginal fistula treatment market is being driven by rising cases of obstetric injuries, inflammatory bowel diseases, and pelvic surgeries.
- Based on the fistula type, the rectovaginal fistula segment is growing at a high rate and is projected to dominate the market.
- On the basis of diagnosis method, the physical examination segment is projected to swipe the largest market share.
- In terms of treatment type, the surgical management segment is expected to dominate the market.
- Based on the end user, the hospitals segment is expected to dominate the market.
- By region, North America is expected to dominate the global market during the forecast period.
Rectal Vaginal Fistula Treatment Market: Dynamics
The rectal vaginal fistula treatment market is shaped by a complex interplay of factors that drive its growth, pose limitations, create new avenues, and present hurdles. Understanding these dynamics is crucial for stakeholders navigating this specialized healthcare segment.
Key Growth Drivers
- Rising Incidence of Conditions Leading to Fistulas: The increasing prevalence of conditions such as inflammatory bowel diseases, particularly Crohn's disease, and complications arising from childbirth (e.g., obstetric trauma, prolonged labor, third- and fourth-degree lacerations) are significant drivers. Additionally, a rise in pelvic cancers and radiation therapy for these cancers also contributes to the formation of rectovaginal fistulas, thereby increasing the patient pool requiring treatment.
- Advancements in Medical Technology and Surgical Techniques: Continuous innovation in surgical approaches, including the development of minimally invasive procedures like laparoscopic repair, offers improved patient outcomes, reduced recovery times, and fewer complications. The advent of novel biomaterials, biological plugs, and regenerative therapies such as stem cell applications and bioengineered scaffolds also enhances treatment efficacy and expands the range of therapeutic options available.
- Increasing Awareness and Education: Growing awareness among women about pelvic health issues, coupled with public health campaigns and improved diagnostic facilities, leads to earlier diagnosis and timely intervention. This increased awareness not only improves patient outcomes but also drives the demand for rectovaginal fistula treatments.
- Improved Healthcare Infrastructure and Expenditure: Investments in modernizing healthcare facilities, particularly in developing countries, and a general rise in healthcare expenditure globally, contribute to better accessibility and availability of advanced treatment options. This facilitates a larger number of patients seeking and receiving appropriate care.
Restraints
- High Cost of Treatment: Advanced surgical procedures, specialized medical devices, and post-operative care for rectovaginal fistulas can be expensive. This high cost can be a significant barrier for patients, especially in regions with limited insurance coverage or lower per capita income, potentially hindering market growth.
- Lack of Awareness and Underdiagnosis in Developing Regions: Despite the prevalence of conditions that can lead to fistulas, there remains a substantial gap in recognizing and adequately diagnosing rectovaginal fistulas, particularly in many developing countries. Cultural stigma surrounding pelvic floor disorders and limited access to specialized medical care contribute to underdiagnosis, preventing many from seeking necessary treatment.
- Shortage of Skilled Professionals: The treatment of rectovaginal fistulas requires specialized surgical skills and expertise. A scarcity of trained healthcare professionals, particularly in rural or underserved areas, can limit the availability and quality of treatment, thereby restraining market expansion.
Opportunities
- Emergence of Regenerative Medicine and Biologics: The ongoing research and development in regenerative medicine, including stem cell therapy and the use of biologic materials, offer promising avenues for more effective and less invasive treatment options. These innovations have the potential to significantly improve healing rates and reduce recurrence, creating substantial market opportunities.
- Focus on Minimally Invasive Techniques: The increasing preference for minimally invasive surgical techniques due to benefits such as smaller incisions, reduced pain, shorter hospital stays, and faster recovery times presents a significant opportunity. Continuous advancements in laparoscopic and robotic-assisted surgical platforms will likely drive this segment of the market.
- Growth in Medical Tourism: Countries with advanced healthcare facilities and lower treatment costs can attract patients from regions where specialized treatment is either unavailable or prohibitively expensive. This growing trend of medical tourism offers an opportunity for specialized centers to expand their patient base and revenue.
- Strategic Collaborations and Investments: Mergers, acquisitions, and strategic partnerships among pharmaceutical companies, medical device manufacturers, and healthcare providers can combine resources, expertise, and technologies. Such collaborations can accelerate research and development, facilitate market expansion, and enhance the development of comprehensive treatment solutions.
Challenges
- High Recurrence Rates and Treatment Complexity: Despite advancements, rectovaginal fistulas can be challenging to treat, and recurrence rates remain a concern, especially for complex fistulas or those caused by underlying conditions like Crohn's disease. The intricate anatomy of the pelvic region and the varied etiologies of fistulas contribute to the complexity of successful repair, demanding multiple interventions in some cases.
- Stigma and Psychological Impact: The sensitive nature of rectovaginal fistulas often leads to significant psychological distress, embarrassment, and social isolation for affected individuals. This stigma can delay diagnosis and treatment-seeking, as patients may be hesitant to discuss their condition, thereby posing a challenge to early intervention and overall market growth.
- Lack of Standardized Treatment Protocols: The absence of universally standardized treatment protocols for all types and etiologies of rectovaginal fistulas can lead to variations in care and potentially suboptimal outcomes. Developing and implementing more consistent guidelines could improve treatment efficacy but remains a challenge given the diverse nature of these conditions.
- Infection and Complications: The risk of infection and other post-operative complications remains a challenge in rectovaginal fistula repair. The proximity of the surgical site to fecal matter and the delicate nature of the tissues involved increase the likelihood of complications, which can impact treatment success and patient recovery.
Rectal Vaginal Fistula Treatment Market: Report Scope
This report thoroughly analyzes the Rectal Vaginal Fistula Treatment Market, exploring its historical trends, current state, and future projections. The market estimates presented result from a robust research methodology, incorporating primary research, secondary sources, and expert opinions. These estimates are influenced by the prevailing market dynamics as well as key economic, social, and political factors. Furthermore, the report considers the impact of regulations, government expenditures, and advancements in research and development on the market. Both positive and negative shifts are evaluated to ensure a comprehensive and accurate market outlook.
| Report Attributes | Report Details |
|---|---|
| Report Name | Rectal Vaginal Fistula Treatment Market |
| Market Size in 2023 | USD 533.65 Million |
| Market Forecast in 2032 | USD 956.61 Million |
| Growth Rate | CAGR of 6.7% |
| Number of Pages | 170 |
| Key Companies Covered | Cook Medical, Takeda Pharmaceutical Company, Johnson & Johnson Services Inc., Pfizer Inc., Allergan, AbbVie Inc, Novartis International AG, Bayer AG, Bristol-Myers Squibb, Boehringer Ingelheim GmbH, Hoffmann-La Roche, Eli Lilly and Company, GlaxoSmithKline plc, Sanofi S.A |
| Segments Covered | By Fistula Type, By Diagnosis Method, By Treatment Type, By End User, and By Region |
| Regions Covered | North America, Europe, Asia Pacific (APAC), Latin America, Middle East, and Africa (MEA) |
| Base Year | 2023 |
| Historical Year | 2018 to 2023 |
| Forecast Year | 2024 to 2032 |
| Customization Scope | Avail customized purchase options to meet your exact research needs. Request For Customization |
Rectal Vaginal Fistula Treatment Market: Segmentation Insights
The global rectal vaginal fistula treatment market is divided by fistula type, diagnosis method, treatment type, end user, and region.
Segmentation Insights by Fistula Type
Based on fistula type, the global rectal vaginal fistula treatment market is divided into rectovaginal fistula, colovaginal fistula, and vesicovaginal fistula.
Rectovaginal Fistula is the most dominant segment within the broader rectal vaginal fistula treatment market. This type of fistula involves an abnormal connection between the rectum (the lower part of the large intestine) and the vagina. The high prevalence of rectovaginal fistulas is largely attributed to injuries sustained during childbirth, such as severe perineal tears that extend to the bowel or infections following an episiotomy. Inflammatory bowel diseases, particularly Crohn's disease, represent the second most common cause, where chronic inflammation can lead to the formation of such fistulas. Additionally, pelvic cancers and radiation therapy for these cancers can also lead to rectovaginal fistula development. Due to its frequent occurrence and the distressing symptom, it causes, rectovaginal fistula treatment forms the core of this market, driving significant research into surgical and non-surgical repair techniques.
Vesicovaginal Fistula constitutes another significant segment. This type of fistula involves an abnormal connection between the bladder (vesico) and the vagina. While distinct from rectovaginal fistulas in the organs involved, vesicovaginal fistulas are also highly prevalent globally, particularly in developing countries due to prolonged and obstructed labor, and in developed countries primarily as a complication of pelvic surgeries, especially hysterectomies. The symptoms involve continuous leakage of urine from the vagina, which severely impacts a woman's quality of life. Treatment often involves surgical repair, though small fistulas might heal with conservative management. The substantial patient population suffering from vesicovaginal fistulas ensures it remains a prominent and well-addressed segment within the market for vaginal fistula treatments.
Colovaginal Fistula is a less common type of fistula within this market segmentation. A colovaginal fistula forms an abnormal connection between the colon (a higher part of the large intestine, beyond the rectum) and the vagina. These are typically rarer than rectovaginal or vesicovaginal fistulas and often arise from different etiologies, such as diverticular disease, inflammatory bowel disease, complications from abdominal surgeries, or certain malignancies. Because of its lower incidence compared to rectovaginal and vesicovaginal fistulas, the colovaginal fistula treatment segment represents a smaller portion of the overall market. However, treatment remains critical due to the severe symptoms and potential for infection and discomfort.
Segmentation Insights by Diagnosis Method
On the basis of diagnosis method, the global rectal vaginal fistula treatment market is bifurcated into imaging techniques, physical examination, and endoscopy.
Physical Examination is often the initial and most dominant diagnostic method in the rectal vaginal fistula treatment market. A thorough physical examination, including a pelvic exam with speculum and a rectovaginal examination, is typically the first step taken by healthcare providers. In many cases, especially for larger or more superficial fistulas, the opening may be visually identified or palpated during this examination. The physical exam also allows the clinician to assess for signs of inflammation, infection, or associated conditions. Its widespread accessibility, low cost, and immediate results make it the primary tool for initial suspicion and preliminary diagnosis, guiding the need for further, more specialized tests.
Imaging Techniques represent the second most significant segment in diagnosing rectovaginal fistulas, particularly for complex or elusive cases. These techniques provide detailed anatomical information that may not be apparent during a physical examination. Magnetic Resonance Imaging (MRI) is considered the gold standard for evaluating rectovaginal fistulas due to its excellent soft-tissue contrast, allowing for precise visualization of the fistulous tract, its relationship to surrounding structures (like the anal sphincter muscles), and the presence of any associated abscesses or secondary tracts. Other imaging modalities include Computed Tomography (CT) scans, which can help locate a fistula and identify its cause, and contrast studies (like fistulograms or barium enemas) that involve injecting dye to trace the fistula's path. These advanced imaging techniques are crucial for surgical planning, as they provide a comprehensive roadmap for repair and help reduce recurrence rates.
Endoscopy plays a vital, albeit often complementary, role in the diagnosis of rectovaginal fistulas, placing it third in terms of market dominance for diagnosis. Endoscopic procedures, such as flexible sigmoidoscopy or colonoscopy, involve inserting a thin, flexible tube with a camera into the rectum and colon to visualize the mucosal lining and potentially identify the internal opening of the fistula. Similarly, cystoscopy can be used to examine the bladder for vesicovaginal fistulas. Endoscopy is particularly valuable when an inflammatory bowel disease, such as Crohn's disease, is suspected as the underlying cause, as it allows for direct visualization of mucosal changes and tissue biopsies. While it can sometimes identify the fistula, its primary strength lies in assessing the health of the surrounding bowel and ruling out other pathologies, thus aiding in comprehensive patient management.
Segmentation Insights by Treatment Type
Based on treatment type, the global rectal vaginal fistula treatment market is divided into conservative management and surgical management.
Surgical Management is by far the most dominant segment in the rectal vaginal fistula treatment market. For the vast majority of rectovaginal fistulas, particularly those that are symptomatic, larger, or not healing spontaneously, surgical intervention is the definitive treatment. The goal of surgery is to close the abnormal connection and restore normal anatomy and function. Various surgical techniques exist, ranging from simple primary repair (direct closure of the fistula opening) for smaller, straightforward fistulas, to more complex procedures involving tissue grafts (e.g., muscle, skin, or rotational flaps from the vagina or rectum) for larger, recurrent, or more complicated fistulas. Minimally invasive approaches like laparoscopic or robotic-assisted surgery are also gaining traction due to their benefits in terms of recovery. The complexity and specialized nature of these procedures, coupled with their necessity for long-term resolution, make surgical management the primary driver and largest component of the market.
Conservative Management represents a smaller but important segment, typically reserved for very small, asymptomatic fistulas, or as a temporary measure before definitive surgical repair. This approach focuses on supportive care to promote spontaneous closure and manage symptoms. It often involves measures such as bowel rest, a low-residue diet, antibiotics to prevent infection, and sitz baths for hygiene. In some cases, biological glues or fibrin sealants may be used to try and close the fistula non-surgically, although their success rates can vary. Conservative management is particularly employed in scenarios where the fistula is very small, or when the patient's underlying health condition (e.g., active inflammation in Crohn's disease) makes immediate surgery unfeasible. While it offers a less invasive option, its limited applicability to certain fistula types and variable success rates mean it accounts for a smaller share of the overall treatment market compared to surgical interventions.
Segmentation Insights by End User
On the basis of end user, the global rectal vaginal fistula treatment market is bifurcated into hospitals, ambulatory surgical centers, and specialty clinics.
Hospitals constitute the most dominant end-user segment in the rectal vaginal fistula treatment market. This dominance is primarily due to the comprehensive range of services they offer, including advanced diagnostic facilities, state-of-the-art surgical theaters, and critical post-operative care units. Rectal vaginal fistula repair, especially for complex or recurrent cases, often requires multidisciplinary teams involving colorectal surgeons, gynecologists, and sometimes urologists or plastic surgeons. Hospitals are uniquely equipped to handle such intricate procedures, manage potential complications, and provide the extensive inpatient care sometimes necessary for recovery. The presence of specialized medical professionals and the ability to perform a wide array of surgical techniques, from open procedures to advanced laparoscopic and robotic-assisted surgeries, solidify hospitals' leading position in this market.
Ambulatory Surgical Centers (ASCs) represent a growing segment in the delivery of rectal vaginal fistula treatment, although they are less dominant than hospitals. ASCs are increasingly preferred for less complex surgical procedures due to their cost-effectiveness, shorter waiting times, and reduced risk of hospital-acquired infections. With the continuous advancement of minimally invasive surgical techniques, some straightforward rectovaginal fistula repairs can now be safely performed in an outpatient setting. This trend allows patients to undergo procedures and return home on the same day, enhancing convenience and reducing overall healthcare costs. The expansion of ASCs and the increasing comfort of surgeons performing certain procedures outside of traditional hospital environments contribute to the growth of this segment.
Specialty Clinics also play a significant, albeit typically more focused, role in the rectal vaginal fistula treatment market. These clinics often specialize in specific medical areas such as urogynecology, proctology, or pelvic floor disorders. They provide highly specialized care, personalized treatment plans, and often foster a more intimate and continuous patient-provider relationship. Specialty clinics frequently serve as initial consultation points for diagnosis and conservative management, and they may perform less complex surgical interventions. For more intricate cases, these clinics often collaborate closely with hospitals, referring patients for advanced surgical procedures while continuing to provide follow-up care. Their growing number and emphasis on specialized expertise are driving an increase in their market share, particularly for initial evaluations and ongoing management.
Rectal Vaginal Fistula Treatment Market: Regional Insights
- North America is expected to dominates the global market
North America holds the dominant position in the rectal vaginal fistula treatment market. This is primarily due to its advanced healthcare infrastructure, high healthcare expenditure, and a significant prevalence of conditions contributing to fistula formation, including Crohn's disease and complex childbirth. The region also benefits from a favorable regulatory environment and substantial investments in research and development, fostering the adoption of cutting-edge technologies and innovative treatment solutions. The presence of numerous key market players actively involved in developing and promoting novel therapies further strengthens North America's leading role in the market.
Europe follows as the second-largest market for rectal vaginal fistula treatment. The region boasts a well-established healthcare system and considerable healthcare spending, which contribute to widespread awareness and access to treatment for rectovaginal fistulas. Countries such as Germany, the UK, and France are at the forefront within Europe, showcasing robust market shares due to their advanced medical facilities and increasing adoption of effective treatment modalities. The emphasis on research and development, coupled with a focus on improving patient outcomes, continues to drive market growth across the European continent.
The Asia Pacific region is rapidly emerging as a significant market for rectal vaginal fistula treatment and is anticipated to exhibit substantial growth. This growth is fueled by increasing awareness of pelvic health issues, continuous improvements in healthcare infrastructure, and a rising trend in medical tourism, particularly in countries like India and Thailand. Governments in developing economies within this region are making considerable investments to modernize their healthcare facilities, thereby enhancing access to treatment and fostering a growing demand for effective rectovaginal fistula management. The increasing prevalence of conditions like Crohn's disease and obstetric complications also contributes to the expanding market in Asia Pacific.
Latin America presents a growing market for rectal vaginal fistula treatment, driven by an increased understanding of gynecological health and a rising incidence of obstetric complications. Policies and initiatives aimed at improving women's healthcare rights and accessibility to treatment options are positively impacting the market in this region. Countries like Brazil are leading the way with significant healthcare infrastructure and growing awareness, while government initiatives in Mexico are also contributing to addressing rectovaginal fistula cases. The demand for specialized treatments and surgical interventions is on the rise, reflecting a growing recognition of this medical challenge across Latin America.
The Middle East and Africa region currently holds the smallest share in the global rectal vaginal fistula treatment market. However, there is a gradual increase in market activity due to growing government initiatives focused on improving the healthcare sector. While the market is less developed compared to other regions, efforts to enhance healthcare infrastructure and increase awareness about women's health issues are expected to contribute to future growth. The Middle East segment, in particular, is anticipated to hold a larger share within this region, driven by ongoing investments in healthcare facilities and services.
Rectal Vaginal Fistula Treatment Market: Competitive Landscape
The report provides an in-depth analysis of companies operating in the rectal vaginal fistula treatment market, including their geographic presence, business strategies, product offerings, market share, and recent developments. This analysis helps to understand market competition.
Some of the major players in the global rectal vaginal fistula treatment market include:
- Cook Medical
- Takeda Pharmaceutical Company
- Johnson & Johnson Services Inc.
- Pfizer Inc.
- Allergan
- AbbVie Inc
- Novartis International AG
- Bayer AG
- Bristol-Myers Squibb
- Boehringer Ingelheim GmbH
- Hoffmann-La Roche
- Eli Lilly and Company
- GlaxoSmithKline plc
- Sanofi S.A
The global rectal vaginal fistula treatment market is segmented as follows:
By Fistula Type
- Rectovaginal Fistula
- Colovaginal Fistula
- Vesicovaginal Fistula
By Diagnosis Method
- Imaging Techniques
- Physical Examination
- Endoscopy
By Treatment Type
- Conservative Management
- Surgical Management
By End User
- Hospitals
- Ambulatory Surgical Centers
- Specialty Clinics
By Region
- North America
- U.S.
- Canada
- Europe
- U.K.
- France
- Germany
- Rest of Europe
- Asia Pacific
- China
- Japan
- India
- South Korea
- Rest of Asia Pacific
- Latin America
- Brazil
- Rest of Latin America
- The Middle East and Africa
- GCC Countries
- South Africa
- Rest of Middle East Africa
Frequently Asked Questions
Table Of Content
Inquiry For Buying
Rectal Vaginal Fistula Treatment
Request Sample
Rectal Vaginal Fistula Treatment
